The impact of Coronavirus on kidney dialysis
When the lockdown was lifted, patients hesitated in going back to the hospitals, fearing that they would contract the virus. As a result, they left their medical conditions untreated for long periods, which in some cases proved to be disastrous.
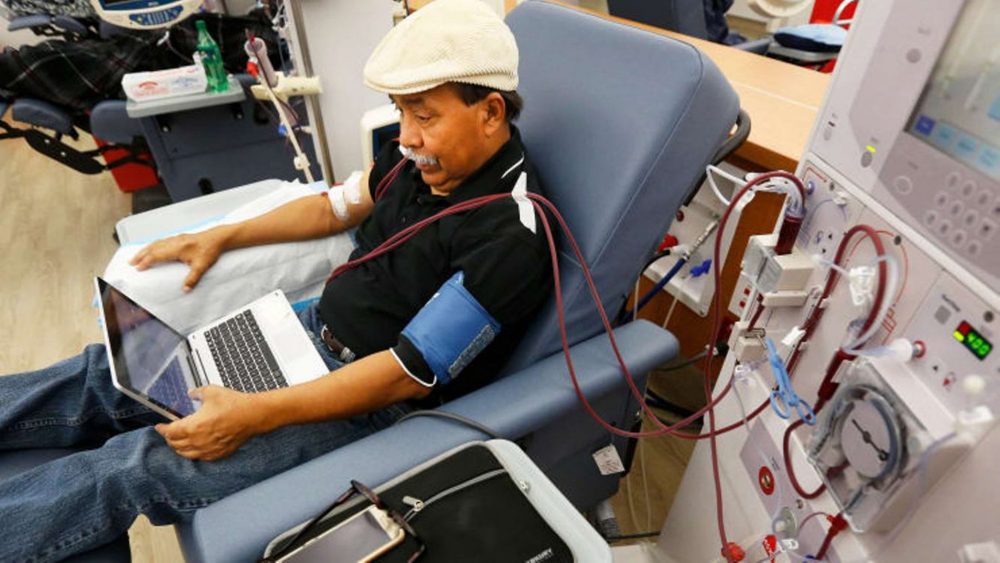
When the Covid-19 pandemic hit India, the entire healthcare industry realigned itself to focus solely on containing the spread of the virus and treating those who had been infected. Resources, energy, and efforts were devoted to tracing, testing, and treating. Amid this, non-communicable diseases – such as diabetes, cancer and cardiovascular diseases took a back seat. When the lockdown was lifted, patients hesitated in going back to the hospitals, fearing that they would contract the virus. As a result, they left their medical conditions untreated for long periods, which in some cases proved to be disastrous.
One such medical morbidity, patients of which have been affected by the pandemic, is chronic kidney disease (CKD), a widespread renal condition which often goes unnoticed and undiagnosed until it is well advanced. A study which assessed the impact of Covid-19 on kidney patients undergoing dialysis stated that over 28% of kidney patients missed one or more dialysis sessions and over 4% stopped reporting for dialysis during the first three weeks of the coronavirus lockdown. This put them at the risk of cardiac arrest (due to the buildup of toxins in their body).
A major cause of mortality, CKD progressively worsens and patients who develop it have to undergo dialysis regularly, a medical process wherein excess water, solutes, and toxins are removed from the blood (since the kidneys can no longer perform these functions naturally). A type of dialysis which is simpler and takes comparatively lesser time (as opposed to Hemodialysis) is ‘Peritoneal Dialysis’(PD). It involves taking the waste out from the body with the help of a cleansing fluid called dialysate which is put into the lining of the belly through a soft catheter. Through this tube, the fluid is then alternately moved in and out of the abdomen thereby drawing out the impurities. What sets this method of dialysis apart is that the patient can themselves dialyze the waste fluid at home about three times a day, with each session lasting around 25-30 minutes. They do not need to go to a hospital or dialysis center.
When Covid cases began emerging in large numbers, hospitals in India transformed themselves into dedicated COVID 19 facilities. Segregated ‘safe’ spaces were created in an attempt to ensure that access to essential services was not hampered. An area of the hospital was cordoned off for those patients who had presented with unavoidable medical conditions such as pregnancies, heart attacks, strokes, blood transfusions and dialysis. However, no protocol was established on how to effectively handle the non-Covid patient influx.
Patients with end stage kidney disease (who mandatorily had to undergo 4-hour sessions thrice a week) began missing their appointments. This caused the toxins to build up in their body and making them feel tired, nauseated and swollen. The high level of potassium in their blood put them at risk for significant heart disease including cardiac arrest. All in all, their situation was dire. Dialysis sessions for most patients became limited, costs at many centres escalated (as technicians and nephrologists had to wear PPE kits and Covid tests had to be done daily) and many could no longer access their medication, as the supply chains had been disrupted. Data from across the world indicated that Chronic Kidney Disease (CKD) patients were at an increased risk of contracting coronavirus and the overall mortality rate of this group of people was also higher.
This brings us to the question – how does this immunocompromised population access necessary treatment while safeguarding itself from the contagious Covid-19? One solution to this overwhelming problem is Peritoneal dialysis (PD), a convenient home-based procedure which can be performed by the patient or any of his/her family member post proper training. It does not put pressure on the heart. While Hemodialysis requires a patient to report to a dialysis center at least three times a day, PD can be done at home, ensuring a better quality of life as toxins are removed from the body regularly. A key factor for the success of PD is patient education and training. Remote patient management technology is another advantage of PD, allowing nephrologists to observe the performance of the therapy on a real time basis. Thus, changes in prescriptions, based on patient needs, can be suggested in a timely manner without one having to come to the clinic.
To ensure that people from all walks of life can access care amid the pandemic, small clinics, and dedicated spaces in small towns for PD need to be created. This will eclipse problems pertaining to space, procuring, and storing of the cleansing fluid and maintenance of routine. To ensure that all people with CKD have access to the same, all Indian state government & UT’s shall include peritoneal dialysis in their plans under Pradhan Mantri National Dialysis Program as it will help states meet the ever-increasing cases of chronic renal failure. All state governments should also have nephrologists enrolled in at least one hospital per major district so that PD can be established on ground via the existing government policy. Additionally, elective kidney surgery (if re-instated) will allow PD to become a life-saving modality of choice.
To conclude, I would like to emphasize on the fact that concerted efforts are needed to address the ever-growing kidney diseases by adopting treatments like peritoneal dialysis, which is high quality, cost-effective, clinically safe, and effective for children, millennials, and elders alike.

