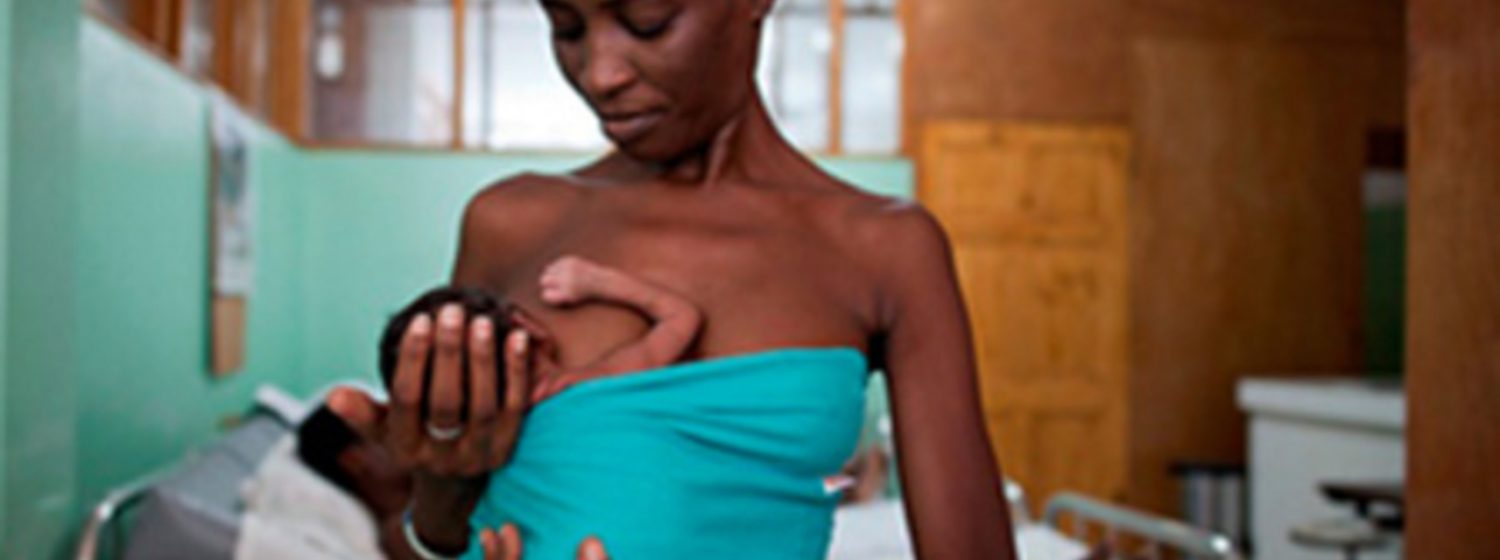
AHO worried about creeping back of Mother-to-Child Transmission of HIV in Africa
In a worrisome trend, mother-to-child transmission of HIV have been creeping back in a handful of countries over the last 18 months—jeopardizing progress in settings that once held the promise of eliminating pediatric AIDS.
This setback has been recorded despite the fact that MTCT rates in hardest-hit countries across sub-Saharan African have dropped steadily over the last decade. Since prevention of MTCT programs began more than 20 years ago, 1.1 million deaths and 2 million infections have been averted among children. Approximately 82% of HIV-positive pregnant women now have access to lifesaving medicines.
Rising MTCT rates require organizations at the front lines of service delivery to take a step back and ask how this happened and how we need to shift course.
Prenatal and postnatal care services are essential in preventing new infections in children, but also serve as a critical service delivery point for women and girls. In 2018, nearly 40% of new diagnoses in Elizabeth Glaser Pediatric AIDS Foundation programs were through service around pregnancy, indicating that quality of care within this timeframe is integral to achieving and sustaining epidemic control.
3 key points highlight concerning trends in MTCT, and opportunities to address critical gaps:
Increasing MTCT and teen pregnancy in Kenya: While Kenya has made substantial progress, between 2015 and 2018 MTCT rates increased from 8.3% to 12.4%. During the same time, teen pregnancies increased 12%, raising questions around how to meet the complex needs of teen mothers with HIV.
Performance gap in low volume sites: EGPAF analysis in Tanzania indicates a significant performance gap between PEPFAR-supported sites and those in the same regions without it. More than 90% of people newly diagnosed in PEPFAR-supported sites were initiated on treatment, compared to less than half in nonsupported sites.
Different countries = different strategies: AHO recently released the first results from a “stacked bar” modelling to determine at what point in pregnancy and breastfeeding new pediatric HIV infections occur, which illustrates the need for tailored strategies to address specific gaps. In Eswatini, more than half of new pediatric infections occurred because HIV-positive women did not receive treatment during pregnancy and breastfeeding. Conversely, in Kenya, nearly half of new pediatric infections occurred because women did not continue treatment throughout pregnancy and breastfeeding. Customized approaches are needed to succeed in unique country contexts.
The complexity of these disparate but related patient dynamics require the global community to redefine MTCT prevention. Providing mothers with lifelong antiretrovirals was a game changer, which in hindsight, led to intensified focus around one aspect of prevention services. Striving for HIV-negative births should not eclipse other goals of comprehensive services, including primary HIV prevention and efforts to meet family planning needs.
To drive programmatic improvement—and reverse increasing infection rates—AHO is mapping the following approaches:
- Improve maternal retesting during pregnancy, labor and delivery, and breastfeeding, particularly in lower prevalence settings.
- Intensify data monitoring to improve tracking of maternal retesting during pregnancy and breastfeeding, follow-up of mother-baby pairs, and maternal and infant outcomes.
- Improve linkage to prevention services for the pregnant and breastfeeding women who test HIV-negative.
- Expand proven youth-friendly pregnancy services to improve health outcomes for young women and babies. Through Kenya’s JUA program, implemented from 2017 – 2019, viral suppression among pregnant adolescents and young mothers increased from 29% to 94%.
- Scale up use of point-of-care early infant diagnosis which has demonstrated effectiveness in reducing median time to return results from 55 days to same-day. There is real opportunity to expand this technology to include viral load monitoring for pregnant and breastfeeding women.
- Expand proven models for intensified follow-up and retention of mother-baby pairs, including established approaches like the community focal mother model.
- Expand male-tailored services, such as Lesotho’s male corner model, which helped increase viral suppression rates among adult men to 87%—compared with 63% nationally.
While each of the above components individually represent important focus areas in our programs, combined they are an opportunity to markedly improve MTCT services.
Increasing rates are another reminder that with HIV, vigilance is essential and complacency begets failure. If we are to maintain progress of the last 3 decades, we must heed this wakeup call and redefine the best ways to prevent MTCT—or risk losing what we’ve gained.

