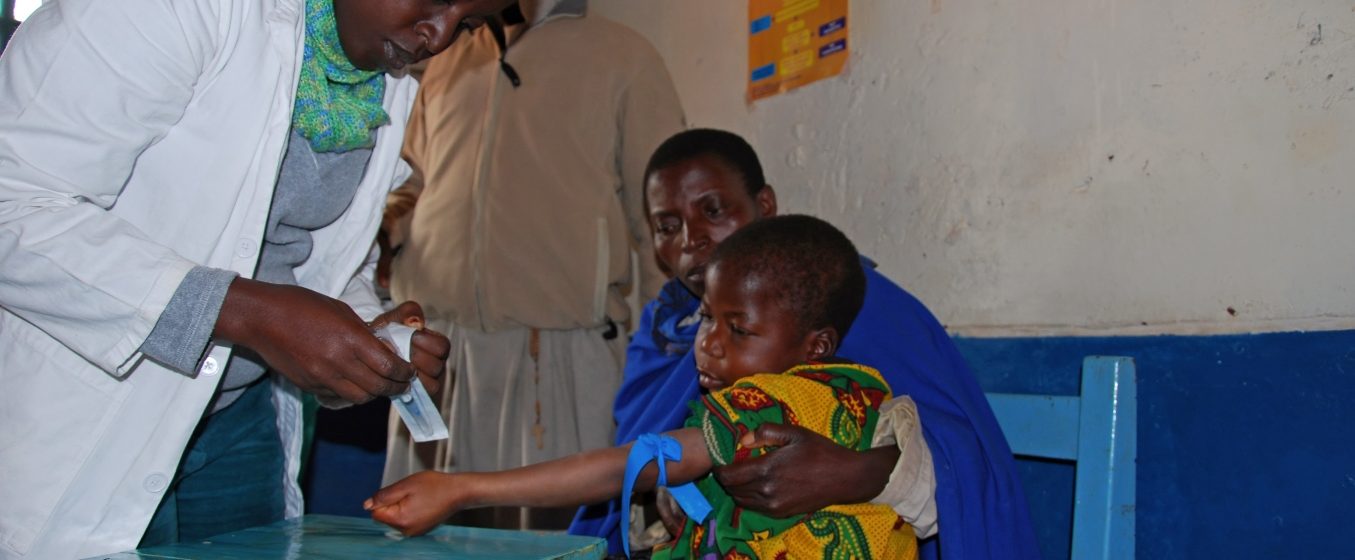


Senegal
Senegal is a country on Africa’s west coast known for its French colonial heritage and natural attractions. Dakar, the capital, features the ancient Médina district and esteemed Musée Théodore Monod, displaying African art. Its population is 14 million people and GDP per capita of USD 1,046.
In contrast to many other countries in sub-Saharan Africa, Senegal’s adult HIV prevalence rate has remained below 1 percent, but is high among key populations: 18.5 percent amongst men who have sex with men and sex workers; and 10.2 percent amongst people who inject drugs. Tuberculosis is highly endemic with an incidence rate of 136 cases per 100,000 population. The most vulnerable populations are those living in overcrowded housing and people living with HIV. Great progress has been achieved to combat malaria and four million bed nets have been distributed in 2014 through a mass campaign. Improving health services’ quality by strengthening health systems is also a priority, including support to health districts for the implementation of an integrated package of services which includes TB, HIV, and malaria, as well as maternal and child health. The government is increasing its efforts to raise domestic financing on health through traditional and innovative partnerships.
AHO PRIORITIES FOR HEALTH DELIVERY PLAN IN SENEGAL
- Administration and management of the AHO, within the framework of the AHO mission and the country’s technical cooperation priorities.
- Universal access to high-quality health services.
- Development of a surveillance system for life expectancy, morbidity, and mortality, and interventions in health promotion and disease prevention.
- Adequate development of sectoral process for the planning, organization, and management of human resources.
Improvement of health and environmental management capacity.
PROGRAMMES & PROJECTS
1. REGULATION, COORDINATION, AND MANAGEMENT OF THE TECHNICAL COOPERATION PROJECTS
PURPOSE
To manage the technical cooperation outlined to address the principal public health problems
EXPECTED RESULTS
- Political and technical management of the cooperative program has contributed to sustainable national and international processes for progress in public health.
- Efficient and timely response to all administrative requirements necessary for the technical cooperation process.
- AHO Office strengthened in its steering role and its ability to address national technical cooperation priorities and respond to them.
2. STRENGTHENING THE PLANNING, ORGANIZATION AND MANAGEMENT OF HUMAN RESOURCES
PURPOSE
To strengthen the capacity of the health authority in the development of essential functions linked to the planning, organization, training, and management of human resources
EXPECTED RESULTS
- Human resources policies executed according to the management and decentralization requirements of the health services.
- Strategic development plan established to educate and train human resources for the analysis, organization, and management of public health.
- Human resources planning, organization and evaluation processes established in the main institutions of the sector.
- Public health research based on the requirements of the new service-delivery models.
3. DEVELOPMENT OF HEALTH SYSTEMS AND SERVICES
PURPOSE
To reduce exclusion in public health, facilitating access to quality services and increasing social benefits in health.
EXPECTED RESULTS
- Legal and regulatory framework established that facilitates the regulatory and control function of the health authority.
- Social security health model defined; proposals developed that allow for more health-related social benefits, primarily for excluded population groups.
- Management models defined and instruments applied that improve the operation of the services network, decision-making processes, budget preparation, and resource allocation.
4. SURVEILLANCE, PREVENTION AND CONTROL OF PRIORITY PROBLEMS IN PUBLIC HEALTH AND DEVELOPMENT OF PUBLIC HEALTH POTENTIAL
PURPOSE
To strengthen national capacity for surveillance, prevention and control of the priority problems in public health, with emphasis on vulnerable groups and the development of public health potential.
EXPECTED RESULTS
- Development, updating and follow-up of public and institutional policies, plans, and legislation in response to priority problems.
- Coordination between programs facilitated and programs functionally integrated into the health services network; strategic partnerships forged with other actors for the production of health and the control of priority problems.
- Collaboration with the process of institution-building at all levels in AHO and other institutions.
- Country able to monitor priority health problems and to adopt the pertinent policies.
- Health worker competencies strengthened in planning, program and project management, epidemiology, promotion, and research at all levels.
- National competencies strengthened along with the capacity to address priority health problems and take advantage of the development potential in border areas.
5. ENVIRONMENTAL HEALTH
PURPOSE
To increase national and local capacity for the identification, prevention, and control of the environmental risk factors that affect health.
EXPECTED RESULTS
- Plans, policies, and the legal framework strengthened to improve the quality of the environment and services.
- Strengthening of environmental health surveillance, covering water, soil and air, as well as the use of hazardous chemical substances and housing quality.
- National and local capacity strengthened for the management of environmental issues and the operation and maintenance of systems and services.
- National strategies for community mobilization, primary environmental care, institutional networks, and inter-sectoral coordination strengthened.
RESOURCES (USD)
AHO SENEGAL 2019 – 2020 (USD million)* based on 2017 pop 15.85 million World Bank
| SO | BUDGET ITEM | AMOUNT* |
| 1 | Combating communicable diseases |
264 |
| 2 | Tackling non communicable diseases |
280 |
| 3 | Addressing determinants of health & risk factors |
250 |
| 4 | Modernising health system and health service |
255 |
| 5 | Improving preparedness, surveillance and response |
260 |
| 6 | Developing good governance & corporate services |
276 |
| Total |
1,585 |
AHO estimates that it needs to spend at least USD100 per capita on health to meet the basic health needs of the people in Africa. This is too far below developed countries e.g. in England it is US$1,300 per capita (2017)

