
Ghana
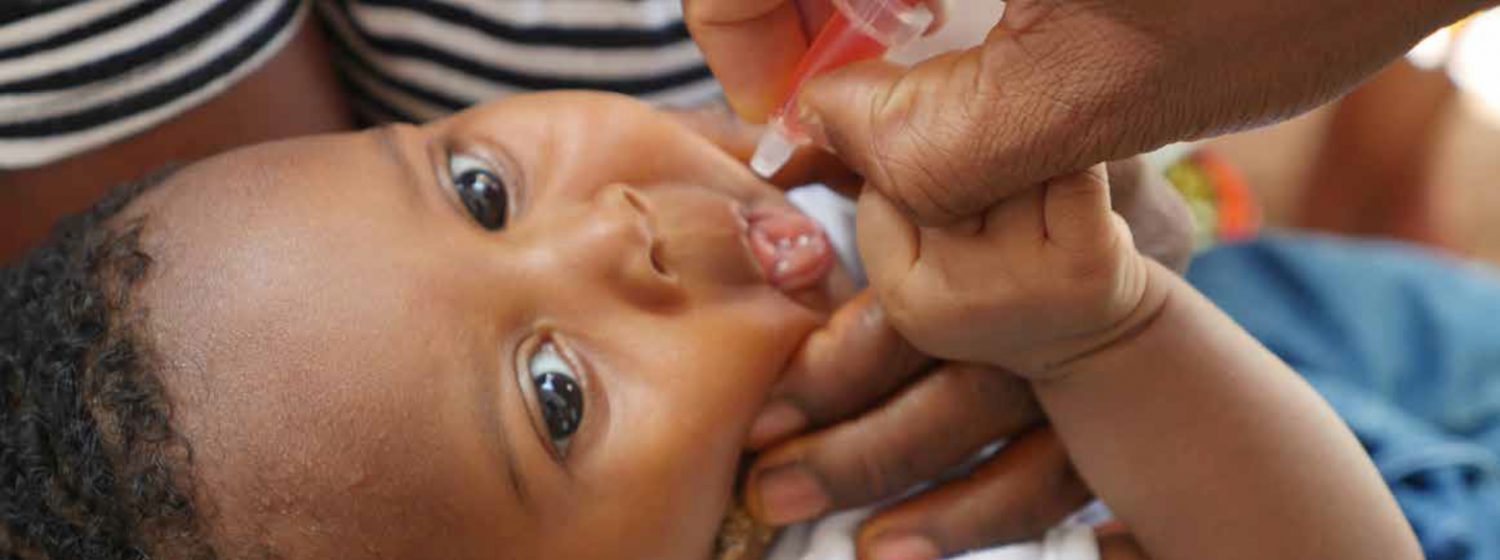
Ghana, a nation on West Africa’s Gulf of Guinea, is known for diverse wildlife, old forts and secluded beaches, such as at Busua. Coastal towns Elmina and Cape Coast contain posubans (native shrines), colonial buildings and castles-turned-museums that serve as testimonials to the slave trade. Its population is 25 million people and GDP per capita of USD 1,858.
Ghana, a lower-middle-income country, was the first country to sign a Global Fund grant in late 2002. The country faces significant challenges from malaria, HIV and TB. Malaria accounts for 8 percent of deaths in the country. Ghana is also one of the countries with the highest burden of multidrug-resistant TB in the world. A recent survey showed that TB prevalence had been underestimated at 71 per 100,000, establishing that the prevalence is now estimated at 264 per 100,000 – a more than 300 percentage difference. In response, Ghana is making robust commits to increase its domestic investments in health. Working with the Global Fund partnership, Ghana has distributed 19 million mosquito nets, and lowered the death rate among children under five due to malaria from 14 percent in 2000 to less than 1 percent in 2012. The country has registered a 43 percent decrease of new HIV infections since 2010, and increased coverage of prevention of mother-to-child transmission coverage from 32 percent to 81 percent. Over 76,000 new tuberculosis cases have been detected and treated.
AHO PRIORITIES FOR HEALTH DELIVERY PLAN IN GHANA
- The Public Health Plan, which includes eight basic points based on national health priorities.
- Resolution of the hospital network crisis.
- Cooperation and coordination between territorial entities.
- Strengthening of the Public Health Surveillance and Information System.
PROGRAMMES & PROJECTS
1. DEVELOPMENT, MANAGEMENT, AND ADMINISTRATION OF AHO
PURPOSE
To have physical and logistical facilities and support personnel to carry out the technical cooperation to the country
EXPECTED RESULTS
- Adequate administrative processes and working conditions in place to meet technical cooperation requirements, as the available resources permit.
2. PREVENTION, CONTROL, AND REDUCTION OF DISEASES
PURPOSE
To strengthen functional groups at the central level and foster coordination with territorial entities on activities to prevent, control, and reduce diseases of importance to public health, with emphasis on priority groups, irrespective of gender, social category, and cultural characteristics, and with a view to reducing injuries and their determinants.
EXPECTED RESULTS
- Epidemiology used by functional groups as an instrument for decision-making and for strengthening prevention, surveillance, and control of communicable diseases of importance to public health, with the aim of helping to attain the indicators.
- Activities carried out by the functional groups in the departments in their areas of specialisation for health promotion and the prevention, surveillance, and control of noncommunicable diseases, with emphasis on those assigned priority.
- Plans consolidated for the prevention, control, and eradication of vesicular and emerging diseases in domestic animals, diseases which jeopardize food production and the international livestock trade.
- Inter-sectoral plans and programs implemented, aimed at understanding the extent of foodborne diseases (FBDs), with this information used in policy-making.
- Programs for the control of endemic zoonoses and emerging and re-emerging diseases implemented, in coordination with relevant entities, including producers.
3. ENVIRONMENTAL HEALTH AND HEALTHY SPACES
PURPOSE
To strengthen national capacity to manage and implement activities for improving sanitary conditions in physical and social environments to better reduce environmental risks that jeopardize the health of the Ghana population.
EXPECTED RESULTS
- Technologies and instruments identified that increase the coverage and quality of water and sanitation services for rural and vulnerable populations.
- Registry of accidents and occupational diseases among the working population strengthened, along with risk assessment and the development of programs to support workers in the informal sector.
- Risk assessment, prevention, and public awareness campaigns strengthened to inform the people about poisoning and environmental pollution from various physical, chemical and biological agents that affect air, soil, and water quality.
- National capacity strengthened through development of the instruments, plans, standards, and information systems proposed for the national environmental health plan, which will allow for implementation of the environmental health program in health and environmental institutions.
- Plans, policies, and programs aimed at making environments healthier implemented through the promotion of healthy lifestyles, sound public policy-making, and the reduction of risks for the vulnerable population.
4. HEALTH INFORMATION
PURPOSE
To strengthen the country’s capacity to generate, analyse, disseminate, and use health information for policymaking in public health administration.
EXPECTED RESULTS
- Development plans for essential public health functions 1 and 2 implemented, and plans corresponding to function.
- Systems created to generate strategic information that will make it possible to anticipate events and better prepare appropriate responses.
- Capacity strengthened to analyse mortality profiles and trends, the disease burden, measurement of inequalities, violence, health situation analysis in primary health care, and disasters.
- Situation rooms developed as a strategic instrument for administrative use at the departmental level. Scientific and technical information and communications processes (database, Virtual Health Library, and Web page) consolidated.
5. FAMILY AND COMMUNITY HEALTH
PURPOSE
To promote public health interventions that improves family and community health throughout the life cycle, with emphasis on child and adolescent health, sexual and reproductive health, and nutrition, by strengthening functional groups at the national, departmental and municipal levels and by supporting the preparation and coordination of sound public policies and strategic partnerships to address the needs of the most vulnerable population groups.
EXPECTED RESULTS
- Critical support strategies implemented for the Strategic Plan for the Expanded Program on Immunization (EPI), to achieve useful vaccination coverage in all departments and municipalities in the country.
- Critical support strategies for plans to eradicate, eliminate, and control vaccine-preventable diseases implemented at the national and/or departmental levels.
- Public policy strategies for sexual and reproductive health (SRH) implemented that strengthen the administrative and epidemiological monitoring of maternal/perinatal health and help reduce maternal mortality at the national, departmental, and local levels.
- SRH activities for the adolescent population initiated, with national support, in priority departments with high reproductive risk.
- Strategic institutional partnerships forged at and with the national and departmental levels that promote legislation to support services for children and adolescents, reorient services for Integrated Management of Childhood Illness (IMCI), and assist caregivers and families.
- Actions and interventions that strengthen the National Plan for Food and Nutrition identified and carried out by functional groups at the national and departmental levels.
- Actions and interventions that strengthen health promotion and access to health services by ethnic minorities identified and carried out.
6. DEVELOPMENT OF AND UNIVERSAL ACCESS TO HEALTH SERVICES
PURPOSE
To strengthen the steering and managerial capacity of health systems and services at the national and departmental levels.
EXPECTED RESULTS
- Decentralised, integrated management models developed in consultation with partners selected on the basis of epidemiological, social, and sanitary priorities.
- Basic health models care based on integrated departmental service networks operating at the central level, with intra-sectoral and inter-sectoral coordination and social participation, and with an emphasis on primary care and community health in five priority departments.
- Public health policies developed for exercising essential public health functions under the supervision of national and departmental health authorities.
- General System for Social Security in Health developed to achieve universal health coverage, quality health services, and a sustainable financial system.
Monitoring and research on the Colombian health system reform process conducted and disseminated
7. HEALTH IN DISASTER AND EMERGENCY SITUATIONS
PURPOSE
To cooperate to improve health and access to services of victims of disasters and humanitarian crises, particularly displaced populations.
EXPECTED RESULTS
- Management of risk and mitigation of the impact of disasters on health strengthened in areas identified as critical by national and local authorities.
- Institutional capacity to respond to the health needs of displaced and vulnerable populations strengthened in departments where AHO has field offices.
Support provided for territorial technical cooperation initiatives
8. SUPPORT FOR NATIONAL HEALTH DEVELOPMENT
PURPOSE
To identify needs and programs and explore opportunities for technical cooperation that are consistent with the guidelines of the National Development Plan and the strategic plans of the Social Protection and AHO.
EXPECTED RESULTS
- Specific cooperation initiatives adopted by AHO in conjunction with its various counterparts periodically evaluated.
- Knowledge and skills required for performing routine functions attained by personnel.
- Effective use by the countries of technical cooperation projects to strengthen institutional capacity in strategic areas, with priority assigned to bordering countries.
RESOURCES (USD)
AHO GHANA BUDGET 2020 (USD million)* based on 2017 pop 28.83 million World Bank
| SO | BUDGET ITEM | AMOUNT* |
| 1 | Combating communicable diseases |
480 |
| 2 | Tackling non communicable diseases |
558 |
| 3 | Addressing determinants of health & risk factors |
450 |
| 4 | Modernising health system and health service |
470 |
| 5 | Improving preparedness, surveillance and response |
475 |
| 6 | Developing good governance & corporate services |
450 |
| Total |
2,883 |
AHO estimates that it needs to spend at least USD100 per capita on health to meet the basic health needs of the people in Africa. This is too far below developed countries e.g. in England it is US$1,300 per capita (2017)

